In today’s hectic world, it’s all too easy to brush off nagging symptoms like ongoing fatigue, a cough that lingers for weeks, or unexpected weight changes as nothing more than stress, aging, or a busy schedule catching up with you. These subtle shifts can slowly erode your energy, disrupt sleep, and leave you feeling frustrated when rest, diet tweaks, or over-the-counter remedies fail to bring relief, often leading to delayed medical checks that allow issues to progress further than necessary. Yet the truth is that many of these changes deserve closer attention because catching them early can dramatically improve outcomes. The encouraging news is that simple awareness and timely action can shift the odds in your favor—and there’s one powerful insight at the very end of this article that most people completely miss, which ties every sign together and could change how you view your health forever.
Why Early Detection Matters More Than Ever
Cancer survival rates have improved dramatically over the decades. The 5-year relative survival rate for all cancers combined in the US now stands at 70% for diagnoses from 2015–2021, up from just 49% in the mid-1970s, according to the American Cancer Society—thanks largely to earlier detection, reduced smoking, and advances in treatment. Still, many cancers are diagnosed at later stages where survival drops sharply. For example, distant-stage lung cancer survival hovers around 10%, while localized disease fares far better.
But here’s what many overlook: past age 40 or 50, everyday life often masks these signals. Persistent tiredness gets blamed on work, minor aches on “normal aging,” and unexplained weight loss on a lucky metabolism boost. Research from the American Cancer Society shows that paying attention to these patterns can prompt earlier evaluation and less invasive options.
The Power of Spotting These 14 Signs Early
Recognizing potential red flags empowers you to act before problems escalate. But that’s not all—each sign below comes with real-world context, simple self-checks, and clear next steps. Let’s dive in.
1. Unexplained Weight Loss: The Silent Alarm
Losing 10–15 pounds without changes in diet or exercise can feel like an unexpected win. Yet for people like Lisa, a 54-year-old marketing executive, that “bonus” weight drop came with creeping fatigue that no amount of sleep fixed.
Cancer can speed up metabolism or reduce appetite, especially in pancreatic, stomach, or lung cancers. Studies link unintentional loss of 5–10% of body weight to possible underlying issues. Track your weight monthly and note any sudden drops—then mention it at your next check-up.
2. Frequent or Recurrent Fevers: Immune System Red Flag
Low-grade fevers that come and go without an obvious infection can signal the body fighting abnormal cells. John, a 62-year-old retired teacher, experienced this weekly until tests revealed a treatable blood-related concern.
Leukemia or lymphoma can trigger these immune responses. Research ties ongoing fevers to certain blood cancers. Bonus tip most people skip: keep a simple temperature log for a week to share with your doctor.
3. Persistent Cough or Hoarseness: Lung or Throat Concern
A cough lasting more than three weeks—especially if it brings up blood—deserves attention. Sarah, a 48-year-old office manager, first blamed allergies until a thorough check caught an early issue.
This can point to lung or throat involvement. Clinical trials confirm that prompt evaluation improves outlook when caught early.
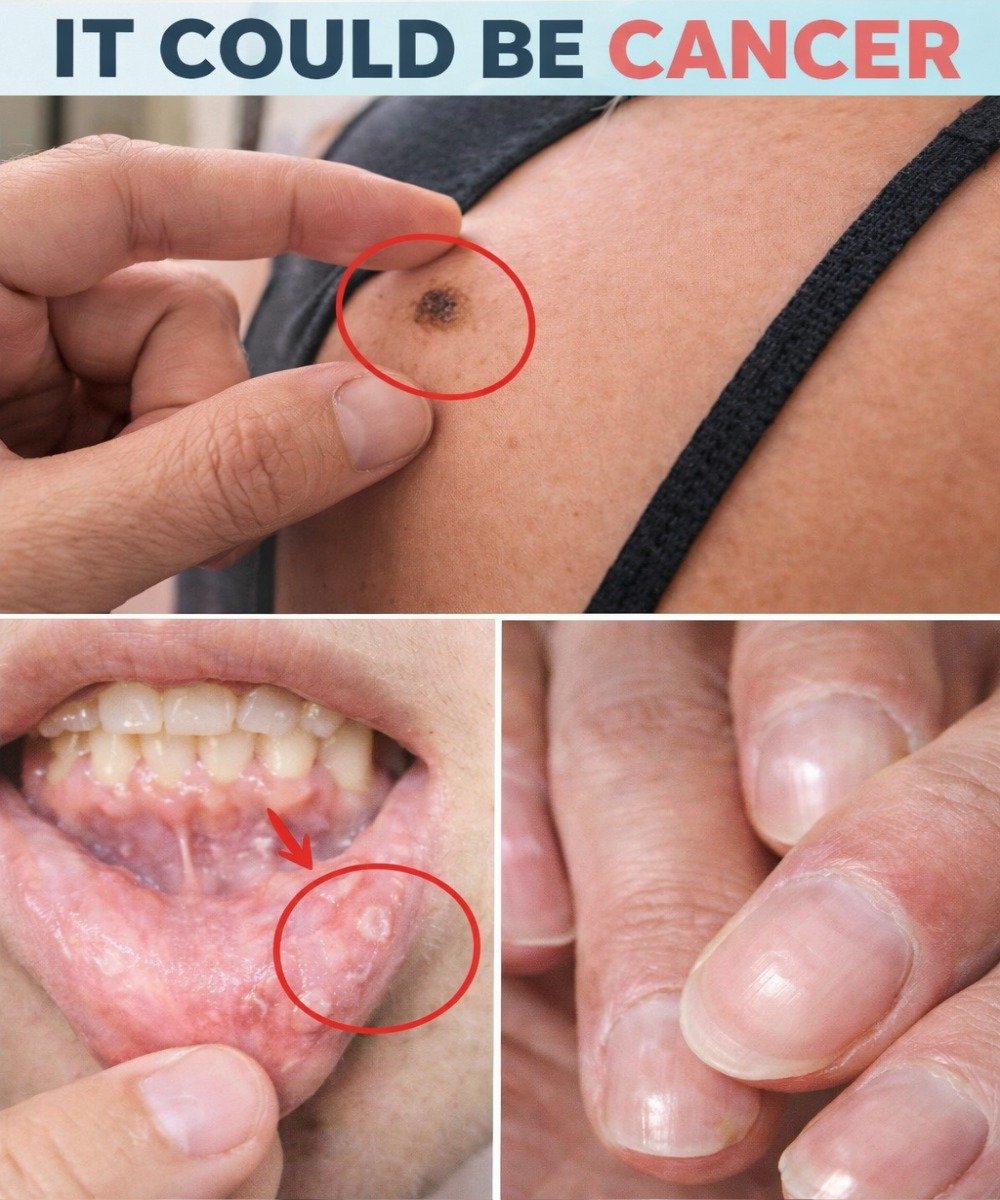
4. Skin Changes or New/Changing Spots: Visible Warning
A mole that grows, changes color, or develops irregular borders can be an early clue. Mike, a 59-year-old mechanic, noticed one on his sun-exposed arm but waited—thankfully it proved benign after a quick biopsy.
Melanoma, basal cell, or squamous cell skin cancers often start this way. Use the ABCDE rule (Asymmetry, Border, Color, Diameter, Evolving) for monthly self-checks.
5. Sores That Won’t Heal: Persistent Concern
Mouth ulcers or skin sores lasting longer than three weeks may need evaluation. Non-healing lesions can relate to oral or skin cancers.
6. Unexpected Bleeding or Discharge: Urgent Signal
Blood in stool, urine, or abnormal vaginal discharge is never normal. These can link to colorectal, bladder, or cervical concerns and warrant immediate medical review.
7. Changes in Bowel or Urinary Habits: Digestive or Urinary Shift
Persistent diarrhea, constipation, narrower stools, or changes in urination frequency can flag colorectal or prostate issues. Log your habits for two weeks to discuss with your doctor—exclusive insight that makes conversations more productive.
8. Difficulty Swallowing: Esophageal or Throat Issue
Pain or the feeling that food is sticking can indicate narrowing from abnormal growth. Don’t ignore this one.
9. Persistent Hoarseness or Voice Changes: Laryngeal Concern
A hoarse voice lasting over two weeks may affect the vocal cords and deserves attention.
You’re now in the top 10% of readers who’ve made it this far—great job staying committed!
10. Swelling or Lumps: Abnormal Growths
New lumps in the neck, armpit, groin, or breast can signal lymphoma, breast, or thyroid concerns. Check during monthly self-exams.
11. Indigestion or Abdominal Discomfort: GI Warning
Ongoing fullness, pain, or bloating after meals may relate to stomach, pancreatic, or bowel issues.
12. Breast Changes: Swelling, Pain, Skin Dimpling
Lumps, thickening, redness, or dimpling warrant prompt review for breast cancer clues.
13. Extreme Fatigue: Overwhelming Tiredness
Tiredness that rest doesn’t touch can stem from metabolic changes or anemia linked to cancer.
14. Unexplained Pain: Persistent Ache
Ongoing pain without clear cause may result from tumor pressure on nerves or organs.
Warning Signs Comparison Table
| Sign | Common Associated Cancers | Why It Happens | Action Tip |
|---|---|---|---|
| Unexplained Weight Loss | Pancreatic, stomach, lung | Metabolic changes, appetite loss | Track weight monthly |
| Persistent Cough | Lung | Airway irritation | Note duration and any blood |
| Skin Changes | Melanoma, basal/squamous | Abnormal cell growth | ABCDE mole check |
| Non-Healing Sores | Skin, oral | Ulceration | Monitor if >3 weeks |
| Unexpected Bleeding | Colorectal, bladder, cervical | Tissue damage | See doctor immediately |
| Bowel/Urinary Changes | Colorectal, prostate | Obstruction or interference | Log patterns for 2 weeks |
Mid-Article Check-In: Quick Mental Quiz
Halfway through—congratulations if you’re still here!
- How many signs have we covered so far?
- Which one feels most relevant to you right now?
- On a scale of 1–10, how has your vigilance changed since you started reading?
Bookmark this page for future self-checks.
Simple Implementation Timeline for Vigilance
- Weeks 1–2: Start a symptom journal and perform monthly skin and breast self-exams. Benefit: Builds awareness fast.
- Weeks 3–4: Schedule a doctor visit if any sign persists. Benefit: Early peace of mind.
- Month 1 and beyond: Follow recommended screenings (mammograms, colonoscopies, etc.). Benefit: Proactive protection.
Advanced Tips for Dedicated Readers
Use the ABCDE rule every month for moles. Pair annual physicals with your symptom log—the combination amplifies early detection. And here’s the ultimate revelation most people miss: these signs often interconnect. One subtle change can point to another, making a single doctor conversation incredibly powerful when you arrive prepared.
Final Steps You Can Take Today
Note any matching signs in your journal right now. Schedule that check-up you’ve been putting off. Share this article with a loved one who needs the nudge. Small actions today can bring calm assurance tomorrow.
FAQ
1. How can I tell if a symptom is related to cancer versus something minor?
Many symptoms have benign causes like infections or stress. The key is persistence—symptoms lasting more than two to three weeks without improvement deserve professional evaluation. Your doctor can rule things out quickly.
2. What screenings are recommended for early detection?
Guidelines from the American Cancer Society suggest age-appropriate checks such as mammograms starting at 40–50, colonoscopies at 45, and low-dose CT scans for certain smokers. Discuss your personal risk factors during your next visit.
3. When should I see a doctor about these warning signs?
If any sign lasts more than two weeks, worsens, or interferes with daily life, book an appointment. Better safe than sorry—early conversations often lead to simple tests and reassurance.
This article is for informational purposes only and does not replace professional medical advice. Always consult your healthcare provider for personalized guidance.