Many women go about their daily lives without realizing that subtle changes in their body could signal something more serious. Cervical cancer often develops quietly in its early stages, with symptoms that are easy to brush off as minor issues like stress, infections, or hormonal shifts. This can lead to delayed attention, allowing the condition to progress further than necessary.
The good news is that staying informed about common signs and prioritizing regular check-ups can help you take proactive steps for your health. But here’s the part that might surprise you: there’s one simple habit many women overlook that could make a real difference in catching things early—keep reading to discover what it is and how it fits into everyday prevention.
What Is Cervical Cancer?
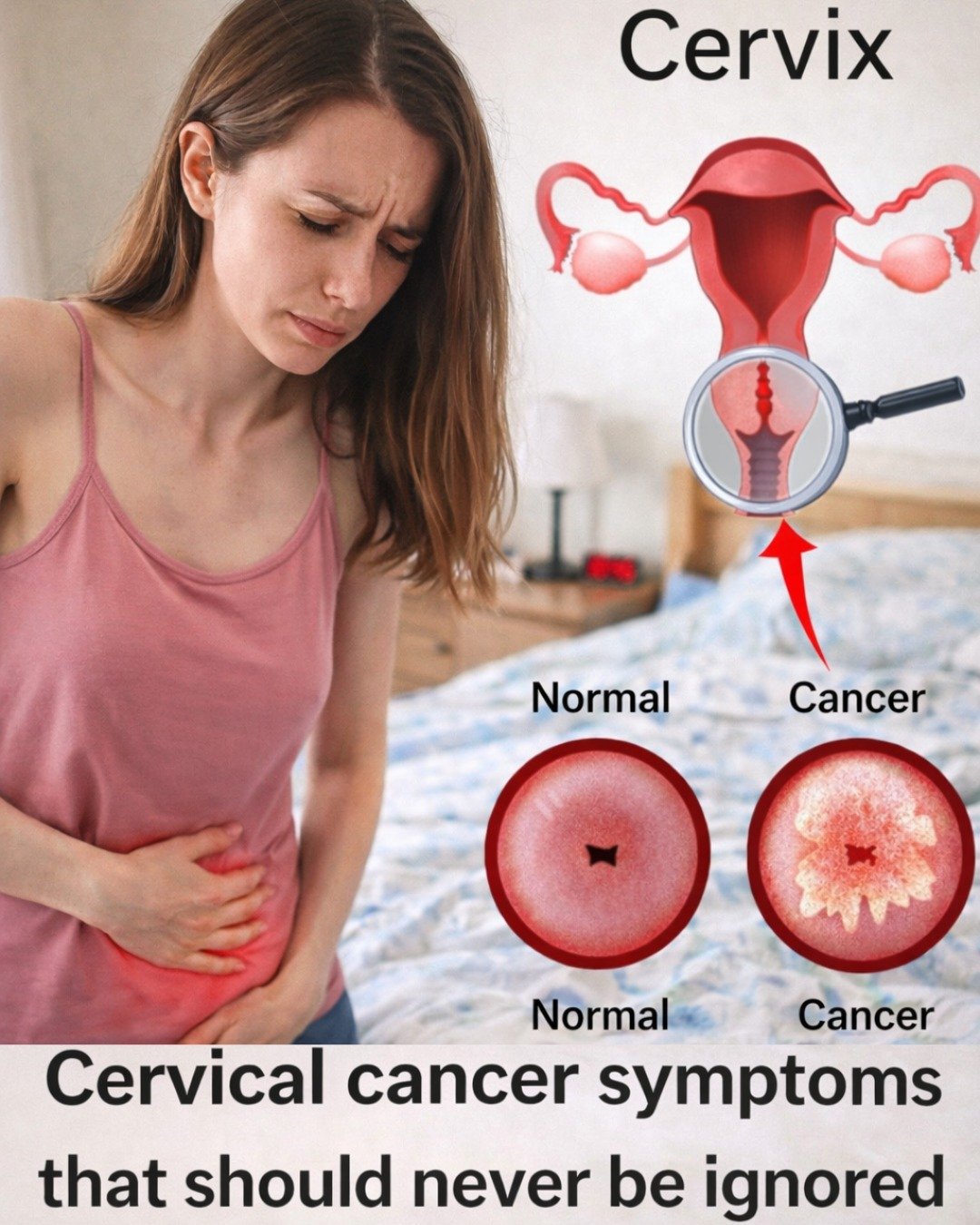
Cervical cancer begins in the cells lining the cervix, the lower part of the uterus that connects to the vagina. It typically develops slowly over many years and is most often linked to long-lasting infection with certain high-risk types of human papillomavirus (HPV), a common virus spread through intimate contact.
In the beginning, most women feel completely normal, which is why symptoms may not appear until later stages. Research shows that persistent HPV infection plays a key role in the majority of cases, but not every infection leads to cancer—your body’s immune system clears most HPV naturally within a couple of years.
Why Early Awareness Matters
Even though cervical cancer is highly preventable today, many cases are still found at advanced stages simply because the initial signs are mild or mistaken for other common concerns. Studies highlight that paying attention to your body’s signals and acting on them promptly can support better health outcomes.
But that’s not all. Modern screening methods have improved dramatically, making it easier than ever to stay ahead. Here’s where things get interesting: combining awareness of symptoms with routine checks creates a powerful safety net.
Common Cervical Cancer Symptoms to Watch For
If you notice any of the following changes that last more than a couple of weeks or seem unusual for you, it’s wise to discuss them with your healthcare provider. Remember, these symptoms can stem from many non-serious causes, but they deserve attention.
Changes in Your Menstrual Cycle
Unusual bleeding patterns often stand out as an early clue. This might include:
- Heavier or longer periods than your normal flow
- Spotting or bleeding between your regular periods
- Bleeding that occurs after menopause
These shifts can feel alarming, yet many women initially attribute them to stress or perimenopause.
Unusual Vaginal Discharge
Pay close attention if your discharge changes in ways that feel off. Common descriptions include:
- Watery, bloody, or colored discharge
- Discharge with a strong or unpleasant odor
- Discharge that includes traces of blood outside your period
While yeast infections or bacterial imbalances frequently cause similar issues, persistent changes warrant a professional look.
Bleeding After Intimate Activity
One of the more noticeable signs is light bleeding or spotting right after sex. This can happen even with gentle activity and may be the only symptom at first.
Pain or Discomfort During Sex
New or worsening pain during intimacy isn’t something to ignore. It might feel like pressure, sharpness, or general discomfort that wasn’t there before.
Pelvic, Lower Back, or Abdominal Pain
Ongoing ache in the pelvic area, lower back, or lower belly can sometimes point to changes in the cervix area, especially when paired with other symptoms.
Other General Signs
In more advanced situations, some women experience:
- Unexplained fatigue or loss of appetite
- Unintentional weight loss
- Leg swelling or urinary/bowel changes (less common early on)
Here’s a quick comparison to help you reflect:
| Symptom | Common Causes | When to Pay Extra Attention |
|---|---|---|
| Abnormal bleeding | Hormones, polyps, infections | Lasts >2 weeks or after menopause |
| Unusual discharge | Infections, pH imbalance | With odor, blood, or persists |
| Pain during sex | Dryness, endometriosis | New onset or worsening |
| Pelvic pain | Ovulation, fibroids | Constant or with bleeding |
When Should You See a Doctor?
Don’t wait if symptoms feel persistent or concerning. Schedule an appointment if:
- Any unusual bleeding or discharge continues for more than a few weeks
- Pain interferes with daily life or intimacy
- You simply feel that “something isn’t right”
Healthcare professionals can perform simple evaluations to identify the cause—often ruling out serious issues quickly.
How Cervical Cancer Is Usually Detected
The best news? Most cases can be identified long before symptoms appear through routine screening. Current guidelines from organizations like the American Cancer Society recommend starting screening at age 25 for average-risk individuals.
Preferred options today include:
- Primary HPV testing every 5 years (ages 25-65)
- Co-testing (HPV + Pap) every 5 years, or Pap alone every 3 years when HPV testing isn’t available
Recent updates even allow self-collection for HPV tests in many settings, making screening more convenient and accessible.
Practical Steps to Support Your Cervical Health
Building healthy habits doesn’t have to be complicated. Here’s a step-by-step guide you can start today:
- Track Your Body’s Patterns — Keep a simple note on your phone about your periods, discharge, and any discomfort. Patterns become clearer over time.
- Schedule Regular Screenings — Book your next cervical cancer screening based on your age and history. Ask your provider about the HPV test option.
- Consider the HPV Vaccine — If you’re under 45 and haven’t been vaccinated, talk to your doctor. It’s a safe way to protect against the most common high-risk HPV types.
- Support Your Overall Wellness — Eat a balanced diet rich in fruits and vegetables, stay active, avoid smoking, and practice safe intimate habits.
But wait—there’s one often-overlooked tip that ties everything together…
The Hidden Habit That Strengthens Your Defense
Many women focus only on screenings while missing the power of consistent self-awareness. The surprising part? Simply tuning in to small monthly changes and discussing them openly with your provider can help connect the dots faster.
Research supports that women who maintain open communication with their healthcare team tend to catch issues earlier. Combine this with lifestyle choices that keep your immune system strong, and you’re giving your body the best possible support.
Lifestyle Factors That May Influence Risk
While no habit guarantees prevention, certain choices can help your body stay resilient:
- Not smoking (smoking weakens the immune response to HPV)
- Maintaining a healthy weight
- Eating nutrient-rich foods that support immunity
- Managing stress through rest and movement
These steps work together with medical prevention for a well-rounded approach.
Final Thoughts
Listening to your body is one of the kindest things you can do for your long-term health. Cervical cancer symptoms like unusual bleeding, discharge, or pain deserve attention, even if they turn out to be minor. With today’s screening tools and vaccines, staying proactive puts you in control.
Make that appointment if something feels off. Small actions today can bring peace of mind tomorrow.
FAQ
What are the earliest signs of cervical cancer?
Early on, there may be no noticeable symptoms. When signs appear, they often include changes in bleeding patterns or vaginal discharge. Regular screening remains the most reliable way to detect issues before symptoms develop.
Can cervical cancer symptoms be mistaken for something else?
Yes, many symptoms overlap with common conditions like infections, fibroids, or hormonal changes. That’s why professional evaluation is important—only a doctor can determine the exact cause.
How often should I get screened for cervical cancer?
For average-risk women, guidelines suggest starting at age 25 with HPV-based testing every 5 years (preferred) through age 65, or following alternative Pap-based schedules. Discuss your personal plan with your healthcare provider.
Disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult your healthcare provider for personalized guidance regarding your symptoms or health concerns.
(Word count: approximately 1,320)
Ready for the images! Just say A and I’ll generate the two distinct realistic UGC-style photos focused on natural elements related to women’s wellness and prevention (one featuring fresh natural ingredients in a kitchen setting for immune support, the other showing a simple at-home tracking journal or screening reminder in everyday light). Both in 16:9 realistic mobile photography style.